This is what COVID-19 looks like through the eyes of nurses on the front lines
[ad_1]
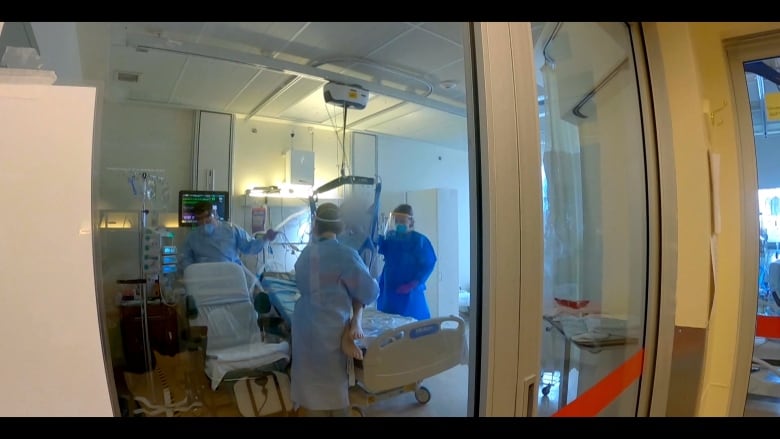
Turning a desperately ill COVID-19 patient onto their stomach may seem simple enough to the uninitiated. It’s not.
In this case, at Quebec City’s Hôpital de l’Enfant-Jésus, it requires a total of seven people crowded around an intensive care bed.
We often hear about how demanding it is for hospital staff and long-term care workers to handle the added workload foisted upon them by the coronavirus pandemic. Here’s just one illustration.
After draping a sheet over the patient, the edges are rolled into the sheet underneath. A pair of pillows are now snug to his chest, and the rolling begins. First, the patient is slid to the edge of the bed. On three, he’s turned to his side. Another three-count, and he is softly delivered onto his stomach.
The room empties. Everyone has work to do.
The Quebec capital has seen a massive spike in coronavirus infections in recent weeks, and a trio of nurses say they’re worried by members of the public trivializing the illness.
To help convince people to take the coronavirus more seriously during the upcoming holidays, they opened their doors to Radio-Canada.
Their names are Cathy Deschênes, Jennifer Boissonnault and Lindsay Vongsawath-Chouinard. Their aim: to show what life in the hot zone looks like.
Each of them agreed to wear a small camera so the public could see how a typical day unfolds. They filmed their colleagues and their patients, and illustrated how the pandemic has made the job harder and more complex.
(scroll up to view the video)

Their point is not to elicit sympathy. As Deschênes says: “It’s difficult, but we love our jobs.”
Instead, they want to show the devastating path some COVID-19 patients are called upon to travel: patients who require more and more staff at their bedside, and need ever larger amounts of treatment time.
And each one of those treatments involves special planning and safety equipment. The ICU rooms have sliding doors, which makes it easier to maintain hot, warm and cold zones. And maintain them, they must.
Each shift has a nurse in charge of making sure the hygiene procedures are being followed and that personal protective equipment, like N95 masks and shields, is worn correctly.
“No one in our department has contaminated themselves (with the virus), we’ve had no outbreaks in intensive care and we’re very proud of that,” Boissonnault says, at one point.
The average age of the COVID-19 patient in the unit is between 60 and 75.
“Some might think that’s old. We don’t think so,” Boissonnault says.
The province has 390 intensive care beds dedicated to COVID-19 patients (20 for pediatric cases), and Enfant-Jésus, in the Maizerets area northeast of downtown Quebec City, accounts for 22 of them.
The unit is not short of business.
Of the 610 COVID-19 patients the hospital has treated so far this year, 90 were in intensive care. And 144 people who entered the hospital with the disease never made it home.
To work in an intensive care unit is to accept that not every patient can be saved, but COVID-19 is rough even for a group of people who must become inured to tragedy.
Public health restrictions mean it’s often not possible for patients’ relatives to be by their bedside, so when things take a turn for the worst, the only hand to hold usually belongs to a nurse, orderly, doctor or other staff member.
At one point, a family is forced to make the devastating decision to halt treatment on their intubated loved one. Two nurses each hold a hand as he is prepared for ‘comfort care’ — palliative measures.
“We’re with you sir,” says Boissonault, holding his left hand. “We’re taking care of you.”
The typical hospital stay for a COVID-19 patient lasts 17 days, but in the ICU sometimes it can stretch to 40 or beyond. Attachments form. When someone dies, there are often tears. There have been weeks when that happens four or five times in just one section of the unit.
People infected with this virus can sometimes take a sudden, catastrophic turn.
“To give comfort to a patient whose family can’t be there with them in their final moments, to be the ones who take their hands in ours during their final moments … it’s troubling,” says Vongsawath-Chouinard, her voice cracking.
So when there is good news, it is celebrated.
Recently, a patient from the Saguenay called Daniel Bouchard made enough progress to be released from the unit to a regular COVID-19 ward in the hospital.

It was his 65th birthday. He had been there eight days, some of them touch-and-go.
The nurses and medical staff got him a card and a small cake. He thanks them in a raspy voice and is overcome with emotion, weeping in his wheelchair as a nurse rubs his shoulders.
“Your tears say a lot,” Boissonnault says.
Safety measures oblige, the gathered staff had to sing Happy Birthday from the next room.
“Thanks so much, you’ve been an all-star team,” Bouchard says.
Minutes later, it is time to leave. Outside the room, scrub-wearing staff line the hall.
They applaud as he is wheeled out of view.
[ad_2]
SOURCE NEWS
